The SSCF has been helping Vascular Services throughout Sussex despite the difficulties of the past two years.
While limited, our achievements have included purchasing an ultrasound scanner for the new Vascular Department at Southlands Hospital in Shoreham. We purchased and donated to Victoria Hospital in Lewes a column lift couch to enable the expansion of services to treat varicose veins. We continue to support NHS staff to improve their knowledge and skills in dealing with Vascular Patient Care by providing bursaries for 3 nurses to attend the South Bank University earlier this year.  We also encourage vascular staff to attend the Annual Vascular Society conference by contributing towards the cost of conference fees.
We also encourage vascular staff to attend the Annual Vascular Society conference by contributing towards the cost of conference fees.
We have managed to do all of this despite fundraising activities having been curtailed and the demands facing our Committee members during the Covid crisis.
As you probably know, all of our Committee members are frontline NHS staff including a number of Consultant Surgeons.
We are looking forward with optimism to 2023 when we hope to resume and active programme of fundraising and ongoing support for Vascular Services throughout Sussex.
In the meantime, we wish all of our supporters a very Merry Xmas and a Happy New Year.

 Very Best wishes to all our supporters for a happy festive season and a joyful 2020
Very Best wishes to all our supporters for a happy festive season and a joyful 2020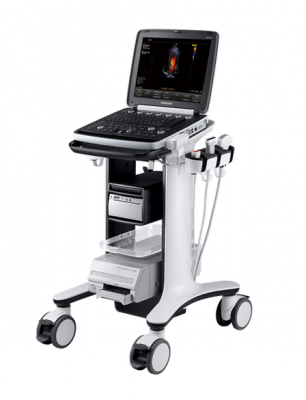




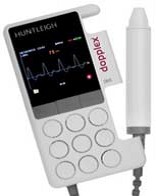 Simon Ward, Consultant Vascular Scientist, asked SSCF for some new hand held doppler machines for nurse specialists, which could be configured to work with laptops to convey the results to the referrer more speedily. The Committee agreed and the new equipment is already up and working in Brighton.
Simon Ward, Consultant Vascular Scientist, asked SSCF for some new hand held doppler machines for nurse specialists, which could be configured to work with laptops to convey the results to the referrer more speedily. The Committee agreed and the new equipment is already up and working in Brighton. We have been able to recruit another new member to our Committee. She is Louise Wilson, currently working as a Vascular Nurse Specialist based in Eastbourne. Louise gratuated from the University of London in 1982 and was Ward Sister on the vascular unit at Charing Cross Hospital from 1988 to 1995. During that time she helped establish the pioneering Vascular Nursing Course at Thames Valley University. Louise was a founding member of the Society of Vascular Nurses and has served on their committee. Louise has been the Vascular Nurse Specialist for East Sussex Hospitals sincer 1988 and has a special interest in the diabetic foot and contributes to the training of podiatrists at the
We have been able to recruit another new member to our Committee. She is Louise Wilson, currently working as a Vascular Nurse Specialist based in Eastbourne. Louise gratuated from the University of London in 1982 and was Ward Sister on the vascular unit at Charing Cross Hospital from 1988 to 1995. During that time she helped establish the pioneering Vascular Nursing Course at Thames Valley University. Louise was a founding member of the Society of Vascular Nurses and has served on their committee. Louise has been the Vascular Nurse Specialist for East Sussex Hospitals sincer 1988 and has a special interest in the diabetic foot and contributes to the training of podiatrists at the